The lack of access to psychedelic integration in Alabama reflects a broader need for learning and growth. Kenton Bartlett, LPC, NCC explores this personal and professional journey in this article. Through research and eduction, psychedelics as medicine are being destigmatized.
Part 1: Searching in Alabama
There were no psychedelic therapists in Alabama.
Or maybe there were, but I couldn’t find them. I Googled, asked, and e-mailed anyone I thought might know someone in Alabama. No one did.
This quest wasn’t something I ever thought I’d undertake.
Early on, I put all drugs in the same category of ‘bad,’ ‘addictive,’ and ‘step one of a downward spiral’. To this day, I’ve never smoked anything or had a beer. As the honor-roll/Eagle-Scout/library-dwelling type, I didn’t want to botch a drug test, poison my brain, or end up in prison, so I stayed far, far away.
Then I read a book.
And several after that.
I soon realized that all drugs were not the same. In fact, it made more sense to call many of them ‘medicines’— defined as compounds used to treat or prevent disease. The more pages I turned, the more I realized how many myths, and straight up lies, I’d internalized as truth.
I learned that when approached with caution and intention, there was an entire class of substances that could yield tremendous therapeutic benefit.
These were psychedelic medicines.
Part 2: Research and Testing
They appealed to me for two reasons.
- I needed help.
As a therapist with too much self-awareness, I sensed that I required something stronger than talk therapy to work through a devastating divorce, some miscellaneous hang-ups, and a melancholy that’s never been far from the foreground.
I’d done as much as I could to tackle these concerns conventionally, but it was time to try something with a better shot at shattering my defenses.
- I wanted to help others.
For seven years, I worked at an eating disorder treatment facility in Alabama. I loved the work we did, and the people I met, but it’s tough to witness such immense suffering, trauma, and relapse and remain unmoved. It started nagging at me that we were missing something; something that might settle these wounds more effectively than the same conversations again and again.
Having learned about these additional tools for dislodging mental stuckness, I felt that the best way to proceed was to learn more myself – through books, research, and personal experience – and see about bringing this approach to our neck of the woods here in Alabama.
Without the guidance of a trained professional, shaman, or psychedelic guide, I was relegated to the path of DIY. It won’t be wise to get into specifics; suffice it to say, I quickly learned what to do and not to do, and how these medicines work.
With some trial and error, I excavated the depths of my psyche and found what I was looking for: healing at a level I doubt would have been possible otherwise.
The altered states themselves were unforgettable. More importantly, however, the resulting life changes have been extraordinary. I’ve been able to access increased self-acceptance, confidence, motivation, meaning, and sense of purpose. I’ve been more in touch with emotions and have been able to engage more openly with friends and family. As someone who was basically an atheist, I’ve felt a newfound connection to spirituality and have a sharper understanding of several concepts I’d previously refuted. I feel more connected to everything, less isolated, less anxious, and more capable of stillness, patience, and peace.
Of course, this isn’t an instant fix, and I’m far from perfect.
But these encounters confirmed everything I’d read, and they reshaped the way I view therapy.
One of these turning points happened at a legal ayahuasca retreat. It was the closest thing to a miracle I’ve ever witnessed. Not only was my own experience life-changing, but in a single weekend over one hundred people with some of the most crushing emotional pain, health conditions, and addictions were able to make breakthroughs that were equally, often more, profound than anything I’d seen in the better part of a decade as a mental health worker in Alabama.
It makes little sense to see these changes, personally and in others, on such an accelerated timeline, and then go back to the old ways of doing things.
Part 3: Learning
To clarify what I mean when I say, ‘this approach,’ I’m referring to any consciousness-altering substance used in a therapeutic context. This includes ketamine, psilocybin (magic mushrooms), MDMA (ecstasy, molly), ayahuasca, DMT, mescaline, LSD, ibogaine, and others.
I’d also like to underline the ample, and growing, body of research that supports my enthusiastic anecdotes.
Ayahuasca, for example, has been shown to help those struggling with eating disorders access the inner compassion that often proves elusive for those stuck in its grips [1, 2]. It’s an invaluable tool for processing grief [3] and has long-lasting, transformative benefits in many areas, including increased spiritual connection, improved relationships, decreased alcohol use and drug dependence, and strengthened sense of self [4].
Ketamine provides fast-acting relief from suicidal ideation (sometimes taking effect within 1-4 hours) and treatment-resistant depression [5, 6, 7]. This medicine generates a response in approximately 70% of those who use it, which is partly why it garners such a high efficacy and safety profile [8]. Ketamine Assisted Psychotherapy (KAP) has been used to treat many conditions, like depression, anxiety, OCD, ADHD, existential distress, relationship issues, bipolar I and II depressive symptoms, and PSTD, and has shown significant improvements of depression and anxiety among all diagnoses, with added notable improvement in those suffering from complex PTSD [9].
MDMA is on its way towards FDA approval and legalization due to its impressive treatment of trauma. After only two to three sessions with traumatized patients, approximately 67% of participants in a well-conducted clinical trial no longer met criteria for PTSD [10]. It’s also been an effective tool in couples therapy to aide in open communication by dialing back the fears and judgments that often stand in the way [11]. Furthermore, a recent study shows promise of MDMA in the treatment of alcohol addiction [12].
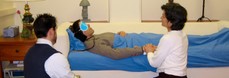
Image of a psychedelic therapy session at Johns Hopkins University using psilocybin.
Psilocybin is expected to fall in line after MDMA for legalization, and it has already been decriminalized in certain parts of the country. It’s been most heavily researched, and proved extraordinary benefit, in reducing end-of-life anxiety and depression in cancer patients [13]. It’s also produced ‘large, rapid, and sustained antidepressant effects in patients with major depressive disorder’ [14]. Moreover, it’s demonstrated stunning potential in the cessation of tobacco, cocaine, alcohol, and other addictions [15, 16, 17].
LSD was a staple in the treatment of numerous psychiatric conditions in the 1950’s, 60’s, and 70’s, before its politically-motivated criminalization, and has exhibited significant power to curb alcohol use after a single session [18].
Ibogaine, a psychoactive substance found in the root bark of a shrub called iboga, is showing promise to be a safe and effective treatment for chemical dependence on alcohol, cannabis, cocaine, and crack [19]. It can also help with withdrawal from heroin and other opiates, often bringing about full detox after a single dose [20].
Part 4: Growing in Alabama & Beyond
I include all this, because I’m trying to boost legitimacy for this topic, and become the person I was looking for: a knowledgeable psychedelic therapist in Birmingham, Alabama who can offer guidance, support, and understanding around these remarkable compounds. To pursue this path, I’ve opened a private practice in Alabama to help others integrate past psychedelic experiences, and offer harm reduction services to mitigate the dangers associated with irresponsible and/or uneducated use. Discussing psychedelics in this way is a legal, ethical, and evidence-based practice that offers significant benefit to society [21].
I’m also working to provide in-person Ketamine Assisted Psychotherapy in Alabama – in collaboration with a prescribing physician – as KAP is the only legal option for a licensed mental health counselor to be present during a psychedelic session at the moment.
While this subject might sound odd to those still operating on the misinformation that I, too, recently believed, it’s my hope that breaking the silence reaches people like you, the reader, who may need to see this.
I equally hope that we all do our part to become educated on this subject, so we can reduce the stigma associated with psychedelics, and support its cautious legalization. Our collective endorsement is the best shot we have at channeling resources into further research and ensuring the availability of these agents for those of us who need them most.
Without exaggeration, these medicines can and do save lives. They can make us better people, living in a better world, when we use them appropriately.
References
AYAHUASCA
1. Lafrance, A., Loizaga-Velder, A., Fletcher, J., Renelli, M., Files, N., & Tupper, K. W. (2017). Nourishing the Spirit: Exploratory Research on Ayahuasca Experiences along the Continuum of Recovery from Eating Disorders. Journal of Psychoactive Drugs, 49(5), 427–435. https://doi.org/10.1080/02791072.2017.1361559
2. Renelli, M., Fletcher, J., Tupper, K. W., Files, N., Loizaga-Velder, A., & Lafrance, A. (2018). An exploratory study of experiences with conventional eating disorder treatment and ceremonial ayahuasca for the healing of eating disorders. Eating and Weight Disorders – Studies on Anorexia, Bulimia and Obesity, 25(2), 437–444. https://doi.org/10.1007/s40519-018-0619-6
3. González, D., Cantillo, J., Pérez, I., Farré, M., Feilding, A., Obiols, J. E., & Bouso, J. C. (2020). Therapeutic potential of ayahuasca in grief: a prospective, observational study. Psychopharmacology, 237(4), 1171–1182. https://doi.org/10.1007/s00213-019-05446-2
4. Harris, R., & Gurel, L. (2012). A Study of Ayahuasca Use in North America. Journal of Psychoactive Drugs, 44(3), 209–215. https://doi.org/10.1080/02791072.2012.703100
KETAMINE
5. Franco, F. M., Lima, A. J. M., & Carol, N. (2021). The effects of the use of ketamine on suicide ideation in patients with treatment-resistant depression. International Journal of Latest Research in Humanities and Social Science, 4(6), 43-47. http://www.ijlrhss.com/paper/volume-4-issue-6/5-HSS-1027.pdf
6. Dadiomov, D., & Lee, K. (2019). The effects of ketamine on suicidality across various formulations and study settings. Mental Health Clinician, 9(1), 48–60. https://doi.org/10.9740/mhc.2019.01.048
7. Andrade, C. (2018). Ketamine for Depression, 6: Effects on Suicidal Ideation and Possible Use as Crisis Intervention in Patients at Suicide Risk. The Journal of Clinical Psychiatry, 79(2), 18f12242. https://doi.org/10.4088/jcp.18f12242
8. Wolfson, P., & Hartelius, G. (2016). The ketamine papers: Science, therapy, and transformation. Multidisciplinary Association for Psychedelic Studies.
9. Dore, J., Turnipseed, B., Dwyer, S., Turnipseed, A., Andries, J., Ascani, G., Monnette, C., Huidekoper, A., Strauss, N., & Wolfson, P. (2019). Ketamine Assisted Psychotherapy (KAP): Patient Demographics, Clinical Data and Outcomes in Three Large Practices Administering Ketamine with Psychotherapy. Journal of Psychoactive Drugs, 51(2), 189–198. https://doi.org/10.1080/02791072.2019.1587556
MDMA
10. Mitchell, J. M., Bogenschutz, M., Lilienstein, A., Harrison, C., Kleiman, S., Parker-Guilbert, K., Ot’alora G., M., Garas, W., Paleos, C., Gorman, I., Nicholas, C., Mithoefer, M., Carlin, S., Poulter, B., Mithoefer, A., Quevedo, S., Wells, G., Klaire, S. S., van der Kolk, B., … Doblin, R. (2021). MDMA-assisted therapy for severe PTSD: a randomized, double-blind, placebo-controlled phase 3 study. Nature Medicine, 27(6), 1025–1033. https://doi.org/10.1038/s41591-021-01336-3
11. Passie, T. (2018). The early use of MDMA (‘Ecstasy’) in psychotherapy (1977–1985). Drug Science, Policy and Law, 4, 205032451876744. https://doi.org/10.1177/2050324518767442
12. Sessa, B., Higbed, L., O’Brien, S., Durant, C., Sakal, C., Titheradge, D., Williams, T. M., Rose-Morris, A., Brew-Girard, E., Burrows, S., Wiseman, C., Wilson, S., Rickard, J., & Nutt, D. J. (2021). First study of safety and tolerability of 3,4-methylenedioxymethamphetamine-assisted psychotherapy in patients with alcohol use disorder. Journal of Psychopharmacology, 35(4), 375–383. https://doi.org/10.1177/0269881121991792
PSILOCYBIN
13. Johnson, M. W., & Griffiths, R. R. (2017). Potential Therapeutic Effects of Psilocybin. Neurotherapeutics, 14(3), 734–740. https://doi.org/10.1007/s13311-017-0542-y
14. Davis, A. K., Barrett, F. S., May, D. G., Cosimano, M. P., Sepeda, N. D., Johnson, M. W., Finan, P. H., & Griffiths, R. R. (2021). Effects of Psilocybin-Assisted Therapy on Major Depressive Disorder. JAMA Psychiatry, 78(5), 481. https://doi.org/10.1001/jamapsychiatry.2020.3285
15. Bogenschutz, M. P., Forcehimes, A. A., Pommy, J. A., Wilcox, C. E., Barbosa, P. C. R., & Strassman, R. J. (2015). Psilocybin-assisted treatment for alcohol dependence: A proof-of-concept study. Journal of Psychopharmacology (Oxford, England), 29(3), 289–299. https://doi.org/10.1177/0269881114565144
16. Johnson, M. W., Garcia-Romeu, A., & Griffiths, R. R. (2017). Long-term Follow-up of Psilocybin-facilitated Smoking Cessation. The American Journal of Drug and Alcohol Abuse, 43(1), 55–60. https://doi.org/10.3109/00952990.2016.1170135
17. Johnson, S., & Black, Q. C. (2020). Classic Psychedelics as a Psychotherapeutic Aid in the Treatment of Stimulant Use Disorder: A Case Report. International Journal of Mental Health and Addiction. https://doi.org/10.1007/s11469-020-00398-7
LSD
18. Fuentes, J. J., Fonseca, F., Elices, M., Farré, M., & Torrens, M. (2020). Therapeutic Use of LSD in Psychiatry: A Systematic Review of Randomized-Controlled Clinical Trials. Frontiers in Psychiatry, 10. https://doi.org/10.3389/fpsyt.2019.00943
IBOGAINE
19. Schenberg, E. E., de Castro Comis, M. A., Chaves, B. R., & da Silveira, D. X. (2014). Treating drug dependence with the aid of ibogaine: A retrospective study. Journal of Psychopharmacology, 28(11), 993–1000. https://doi.org/10.1177/0269881114552713
20. Mash, D. C., Kovera, C. A., Pablo, J., Tyndale, R., Ervin, F. R., Kamlet, J. D., & Lee Hearn, W. (2001). Chapter 8 Ibogaine in the treatment of heroin withdrawal. In The Alkaloids: Chemistry and Biology (pp. 155–171). Elsevier. https://doi.org/10.1016/s0099-9598(01)56012-5
INTEGRATION / HARM REDUCTION
21. Gorman, I., Nielson, E. M., Molinar, A., Cassidy, K., & Sabbagh, J. (2021). Psychedelic Harm Reduction and Integration: A Transtheoretical Model for Clinical Practice. Frontiers in Psychology, 12. https://doi.org/10.3389/fpsyg.2021.645246